Models of Stress

Like many other psychological constructs (for example, personality or intelligence), the construct of ‘stress’ lacks a uniformly accepted definition. Literally, the term was borrowed from physics, in which it referred to a force or mechanical pressure that resulted in strain upon a particular structure. For example, a professional diver creates stress on a diving board in his or her approach to it; the flexibility of the diving board in response to the stress of his or her action represents strain. In this usage, stress leads to strain, with stress serving as a stimulus and strain as the response. This logic, however, has not been consistently followed in the translation of the term ‘stress’ from physics to psychology. Statements like “you are stressing me out” or “my job is causing me a lot of stress,” seem to use the term ‘stress’ as a response rather than a stimulus.
For purposes of clarity, it is probably best to differentiate between the use of the term ‘stress’ to refer to an environmental stimulus and its use to refer to the body’s response to that stimulus. Let’s call stimuli related to stress stressors, and the body’s response to stress the stress response. Given this distinction, events like job stress, traffic jams, interpersonal conflict, being pestered by telemarketers, and daily hassles represent stressors, while autonomic nervous system arousal, insomnia, worry and anxiety, and social withdrawal represent stress responses.
 Although it has been helpful to distinguish stressors as either physical (change in temperature, posture, or physical activity) or psychological (threat to self-esteem or safety) in nature (Lovallo, 1997), the body’s response to them is often quite similar.
Although it has been helpful to distinguish stressors as either physical (change in temperature, posture, or physical activity) or psychological (threat to self-esteem or safety) in nature (Lovallo, 1997), the body’s response to them is often quite similar.
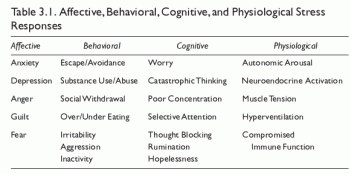
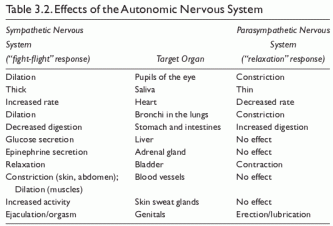
Conceptually, it is useful to differentiate stress responses into physiological, cognitive, affective, and behavioral (see Table 3.1). Physiological responses include the various components of the fight-flight response system of the autonomic nervous system outlined in section 1 in addition to muscle tension, a manifestation of the somatic nervous system. In a synchronized response to a particular stressor, pupils dilate, blood flow is redistributed to the muscles and brain, heart rate increases, respiration rate increases, and the neuroendocrine system releases catecholamines and cortisol into the bloodstream (see Table 3.2).
Neuroendocrine responses lead to a compromised immunologic status, leaving the body less able to resist infection by bacteria, viruses, and fungi (Lovallo, 1997). Cognitive stress responses include increased worry, maladaptive catastrophic thinking, and rumination, coupled with decreased concentration and information processing (blocked thoughts). Depression, anxiety, and anger constitute some affective stress responses, and social withdrawal, behavioral avoidance, substance use and abuse, irritability, and aggression are possible behavioral stress responses.
 It is generally recognized that these various response systems are interrelated in some way so that increases in one response system affect responses in the three remaining systems.
It is generally recognized that these various response systems are interrelated in some way so that increases in one response system affect responses in the three remaining systems.
It is also important to differentiate short-term, or acute, stress responses, from longer-term, or chronic, stress responses. A single stress-filled encounter is extremely unlikely to result in an enduring medical problem like a peptic ulcer, asthma, or cardiovascular disease. As has been widely reported, however, there are recognized associations between life stressors and a variety of chronic medical disease endpoints, including cancer (Anderson, 2002), coronary heart disease (Rozanski, Blumenthal, and Kaplan, 1999), diabetes mellitus (Cox and GonderFrederick, 1991), gastrointestinal disturbances (Duffy et al., 1991; Levenstein, 2002), and skin diseases (House et al., 1979), among others (Caplan et al., 1975; Cobb and Rose, 1973). Because these chronic health problems develop over periods of time as long as years or even decades and the physiological changes that occur during this period occur gradually, it is generally believed that these chronic stress responses evolve from acute stress responses that occur either too frequently or at too great an intensity. In other words, chronic stress responses could be prevented if acute stress responses to environmental stressors never happened in the first place.
The exact mechanism involved in the transition from acute to chronic stress responses is a matter of debate. While some investigators have focused on the causal relations among acute physiological responses and chronic diseases (McEwen and Stellar, 1993), others have highlighted the direct link between various acute behavioral stress responses (for example, smoking or substance use) and chronic diseases (Cohen and Rodriquez, 1995). In the case of cardiovascular disease, for example, exaggerated acute physiological responses (Krantz and Manuck, 1984), acute behavioral responses like smoking and leading a sedentary life (Paffenbarger et al., 1986), and the acute affective response of depression (Rozanski et al., 1999) have all been implicated as factors contributing to the development of atherosclerosis. It is evident in relations like these that multiple causal factors are likely to be involved in explaining how acute stress responses lead to specific chronic stress responses. Several theories regarding the mechanisms responsible for mediating the relation between a psychological construct like stress and actual physiological tissue damage have been examined and have received some empirical support.







